A Patient's Guide to Lumbar Facet Joint Arthritis
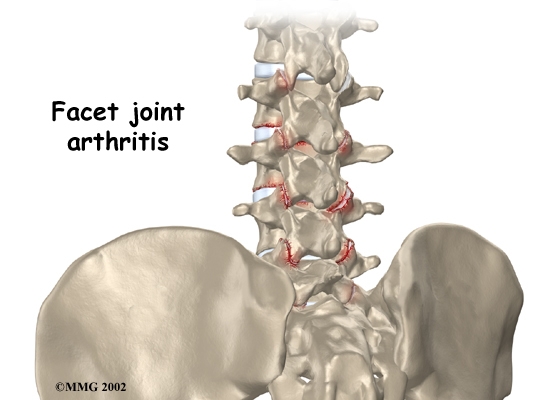
Introduction
Arthritis of the lumbar facet joints can be a source of significant low back pain. Aligned on the back of the spinal column, the facet joints link each vertebra together. Articular cartilage covers the surfaces where these joints meet. Like other joints in the body that are covered with articular cartilage, the lumbar facet joints can be affected by arthritis.
This guide will help you understand
- how the problem develops
- how doctors diagnose the condition
- what treatment options are available
Chiropractic Treatment
Patients are usually seen a few times a week for about 4-6 weeks. In severe and chronic cases, additional treatment may be warranted. Low back pain is the number one reason patients seek care at the Winchester Hospital Chiropractic Center. Facet joint pain and inflammation is one of the common causes of pain in the lower back. Manual treatments such as spinal manipulation have been shown to be one of the most effective in treating people with facet joint pain which causes lower back pain. Chiropractic doctors are the experts in spinal adjustments and manipulation. In fact, chiropractors perform 94% of all spinal manipulations in the United States. Spinal manipulation is one of the only ways to induce motion at specific vertebra in the spine. Chiropractic adjustments help restore normal motion to the joints, reduce pain and inflammation and relieve irritation to the sensitive nerves. Additionally, you will also be shown neutral spinal postures aimed at decreasing pain, improving mobility, strength and function.
Patients are taught how to protect their spines and prevent the problems from returning again. Strengthening exercises are also incorporated. Treatments are often combined with electrical muscle stimulation, ice, ultrasound, exercises, exercise balls, soft tissue massage, and traction. All of these are designed to help decrease pain and inflammation and improve function and mobility. Nutritional recommendations may be prescribed. For example, glucosamine sulfate has been proven effective in not only reducing pain, but in reversing some of the wear in cartilage and actually stimulating new growth of the cartilage. Ginger extract has been shown to have the same clinical effects on pain as does Celebrex.
Anatomy
What part of the back is involved?
The human spine is made up of twenty-four spinal bones, called vertebrae. Vertebrae are stacked on top of one another to create the spinal column. The spinal column gives the body its form. It is the body's main upright support.
The back portion of the spinal column forms a bony ring. When the vertebrae are stacked on top of each other, these bony rings create a hollow tube. This tube, called the spinal canal, surrounds the spinal cord as it passes through the spine. Just as the skull protects the brain, the bones of the spinal column protect the spinal cord.
Between the vertebrae of each spinal segment are two facet joints. The facet joints are located on the back of the spinal column. There are two facet joints between each pair of vertebrae--one on each side of the spine. A facet joint is made of small, bony knobs that line up along the back of the spine. Where these knobs meet, they form a joint that connects the two vertebrae. The alignment of the facet joints of the lumbar spine allows freedom of movement as you bend forward and back.
The surfaces of the facet joints are covered by articular cartilage. Articular cartilage is a smooth, rubbery material that covers the ends of most joints. It allows the bone ends to move against each other smoothly, without friction.
Causes
Why do I have this problem?
Normally, the facet joints fit together snugly and glide smoothly, without pressure. If pressure builds where the joint meets, the cartilage on the joint surfaces wears off, or erodes.
Each segment in the spine has three main points of movement: the intervertebral disc and the two facet joints. Injury or problems in any one of these structures affects the other two. As a disc thins with aging and from daily wear and tear, the space between two spinal vertebrae shrinks. This causes the facet joints to press together.
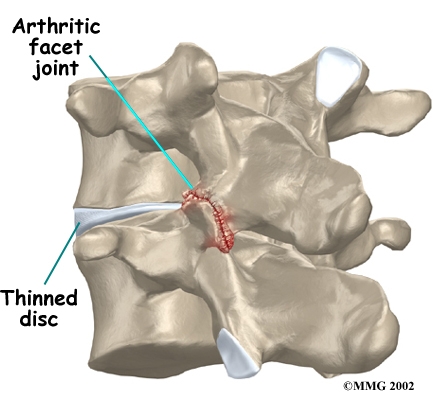
Facet joints can also become arthritic due to a back injury earlier in life. Fractures, torn ligaments, and disc problems can all cause abnormal movement and alignment, putting extra stress on the surfaces of the facet joints.
The body responds to this extra pressure by developing bone spurs. As the spurs form around the edges of the facet joints, the joints become enlarged. This is called hypertrophy. Eventually, the joint surfaces become arthritic. When the articular cartilage degenerates, or wears away, the bone underneath is uncovered and rubs against bone. The joint becomes inflamed, swollen, and painful.
View animation of facet arthritis
Facet joint arthritis develops slowly over a long period of time. This is partly because spinal degeneration in later life is the main cause of facet joint arthritis. Symptoms rarely develop immediately when degeneration is causing the problems. However, rapid movements, heavy twisting, or backward motions in the low back can injure a facet joint, leading to immediate symptoms.
Symptoms
What does the condition feel like?
Pain from facet joint arthritis is usually worse after resting or sleeping. Also, bending the trunk sideways or backward usually produces pain on the same side as the arthritic facet joint. For example, if you lie on your stomach on a flat surface and raise your upper body, you hyperextend the spine. This increases pressure on the facet joints and can cause pain if there is facet joint arthritis.
Pain may be felt in the center of the low back and can spread into one or both buttocks. Sometimes the pain spreads into the thighs, but it rarely goes below the knee. Symptoms of nerve compression--numbness or tingling--are usually not felt because facet arthritis generally causes only mechanical pain. Mechanical pain is pain from abnormal movement in the spine.
However, symptoms of nerve compression can sometimes occur at the same time as the facet joint pain. The arthritis can cause bone spurs at the edges of the facet joint. These bone spurs may form in the opening where the nerve root leaves the spinal canal. This canal is called the neural foramen. If the bone spurs rub against the nerve root, the nerve can become inflamed and irritated. This nerve irritation can cause symptoms where the nerve travels. These symptoms may include numbness, tingling, slowed reflexes, and muscle weakness.
Diagnosis
How do doctors diagnose the problem?
Diagnosis begins with a complete history and physical examination. Your doctor will ask questions about your symptoms and how your problem is affecting your daily activities. This will include questions about where you feel pain and if you have numbness or weakness in your legs. Your doctor will also want to know what positions or activities make your symptoms worse or better.
Then the doctor performs a physical exam to determine which back movements cause pain or other symptoms. Your skin sensation, muscle strength, and reflexes are also tested.
X-rays can show if there are problems in the bone tissue in and near the facet joints. The images can show if degeneration has caused the space between the vertebrae to collapse and may show if bone spurs have developed near the facet joints.
When more information is needed, your doctor may order magnetic resonance imaging (MRI). The MRI machine uses magnetic waves rather than X-rays to show the soft tissues of the body. This test gives a clear picture of the facet joints to see whether they are enlarged or swollen. This machine creates pictures that look like slices of the area your doctor is interested in. The test does not require dye or a needle.
Computed tomography (a CT scan) may be ordered. This is a detailed X-ray that lets your doctor see "slices" of bone tissue. The image can show whether the surface of the joint has eroded and whether bone spurs have developed.
A diagnostic injection may be used to locate the source of pain. The doctor uses a long needle to inject a local anesthetic (numbing medication) into either the joint or into the nerve that goes to the joint. The doctor watches the needle on a fluoroscope to make sure it reaches the correct spot. A fluoroscope is a special X-ray television that allows the doctor to see your spine and the needle as it moves. Once the doctor is sure the needle is in the right place, the medicine and a special dye are injected. The doctor watches the dye to make sure the medication is correctly placed. The results from the injection help the doctor make the diagnosis. If pain goes away, it helps confirm the source of pain.