A Patient's Guide to Thoracic Disc Herniation
Introduction
A rise in the use of MRI (magnetic resonance imaging) has led to the discovery that many people, perhaps as many as fifteen percent of Americans, have a thoracic disc herniation. Seeing a herniated thoracic disc on MRI is often "incidental," meaning it shows up when the person has MRI testing for another problem.
Few people with a herniated thoracic disc feel any symptoms or have any problems as a result of this condition. In rare cases when symptoms do arise, the main concern is whether the herniated disc is affecting the spinal cord.
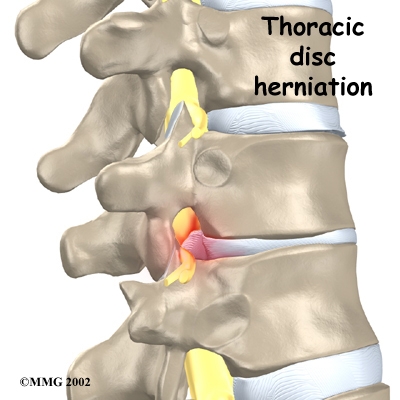
Although people often refer to a thoracic disc herniation as a "slipped disc," the disc doesn't actually slip out of place. Rather, the term "herniation" means that the material in the center of the disc has squeezed out of the normal space. In the thoracic spine, this condition mostly affects people between forty and sixty years old.
This guide will help you understand
- how the problem develops
- how doctors diagnose the condition
- what treatment options are available
Chiropractic Treatment
The chiropractic approach is to help restore a more normal motion and position of affected spinal joints and bones by specific chiropractic adjustments or manipulation. This is often combined with ice, traction, soft tissue massage, electrical muscle stimulation, ultrasound, traction, exercise and stretching. Please see the treatments section for descriptions of each of these procedures. We do not always adjust or manipulate the spine in the presence of certain disc and nerve problems in the mid-back or thoracic spine. Depending on your exam findings, other techniques can sometimes be used. There are very specific therapeutic exercises which have been proven very effective in reducing disc problems in the thoracic spine. These will be discussed at length and demonstrated in the office. Traction can help de-compress the pressure on the discs of mid-back. Electrical muscle stimulation and ice are commonly used to help reduce the inflammation in the muscles and nerves. Longstanding poor posture is a common cause of disc problems in the thoracic spine. Therefore, postural corrective exercises will be prescribed. A thorough chiropractic examination and history will help in identifying the appropriate treatment for you.
Anatomy
What parts of the spine are involved?
The human spine is formed by twenty-four spinal bones, called vertebrae. Vertebrae are stacked on top of one another to create the spinal column. The main section of each vertebra is a round block of bone, called the vertebral body.
The thoracic spine is made up of the middle twelve vertebrae. Doctors often refer to these vertebrae as T1 to T12. The thoracic spine starts at the base of the neck. The lowest vertebra of the thoracic spine, T12, connects below the bottom of the rib cage to the first vertebra of the lumbar spine, called L1.
The upper half of the thoracic spine is much less mobile than the lower section, making disc herniations in the upper thoracic spine rare. Seventy-five percent of thoracic disc herniations occur from T8 to T12, with the majority affecting T11 and T12.
The intervertebral disc is a specialized connective tissue structure that separates the vertebral bodies. The disc is made of two parts. The center, called the nucleus, is spongy. It provides most of the disc's ability to absorb shock. The nucleus is held in place by the annulus, a series of ligament rings surrounding it. Ligaments are strong connective tissues that attach bones to other bones.
Healthy discs work like shock absorbers to cushion the spine. They protect the spine against the daily pull of gravity and during activities that put strong force on the spine, such as jumping, running, and lifting.
The spinal canal is a hollow tube inside the spinal column. It surrounds the spinal cord as it passes through the spine. The spinal cord is similar to a long wire made up of millions of nerve fibers. Just as the skull protects the brain, the bones of the spinal column protect the spinal cord. The spinal canal is narrow in the thoracic spine. Any condition that takes up extra space inside this canal can injure the spinal cord.
Blood vessels that run up and down the spine nourish the spinal cord. However, only one vessel, the anterior spinal artery, goes to the front of the spinal cord in the area between T4 and T9. Doctors call this section of the spine the "critical zone." If this single vessel is damaged, as can happen with pressure from a herniated thoracic disc, the spinal cord has no other way to get blood. Left untreated, this section of the spinal cord dies, which can lead to severe problems of weakness or paralysis below the waist.
Causes
Why do I have this problem?
Thoracic disc herniations are mainly caused by wear and tear in the disc. This wear and tear is known as degeneration. As a disc's annulus ages, it tends to crack and tear. These injuries are repaired with scar tissue. Over time the annulus weakens, and the nucleus may squeeze (herniate) through the damaged annulus. Spine degeneration is common in T11 and T12. T12 is where the thoracic and lumbar spine meet. This link is subject to forces from daily activity, such as bending and twisting, which lead to degeneration. Not surprisingly, most thoracic disc herniations occur in this area.
Less commonly, a thoracic disc may herniate suddenly (an acute injury). A thoracic disc may herniate during a car accident or a fall. A thoracic disc may also herniate as a result of a sudden and forceful twist of the mid-back.
Diseases of the thoracic spine may lead to thoracic disc herniation. Patients with Scheuermann's disease, for example, are more likely to suffer thoracic disc herniations. It appears these patients often have more than one herniated disc, though the evidence is not conclusive.
The spinal cord may be injured when a thoracic disc herniates. First, the spinal canal of the thoracic spine is narrow, so the spinal cord is immediately in danger from anything that takes up space inside the canal. Second, most disc herniations in the thoracic spine squeeze straight back, rather than deflecting off to either side. As a result, the disc material is often pushed directly toward the spinal cord. Third, a herniated disc can cut off the blood supply to the spinal cord. Discs that herniate into the "critical zone" of the thoracic spine (T4 to T9) can shut off blood from the one and only blood vessel going to the front of the spinal cord in this section of the spine. This can cause the nerve tissues in the spinal cord to die, leading to severe problems of weakness or paralysis in the legs.
Symptoms
What does the condition feel like?
Symptoms of thoracic disc herniation vary widely. Symptoms depend on where and how big the disc herniation is, where it is pressing, and whether the spinal cord has been damaged.
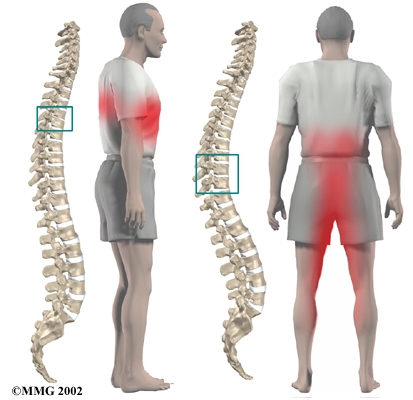
Pain is usually the first symptom. The pain may be centered over the injured disc but may spread to one or both sides of the mid-back. Also, patients commonly feel a band of pain that goes around the front of the chest. Patients may eventually report sensations of pins, needles, and numbness. Others say their leg or arm muscles feel weak. Disc material that presses against the spinal cord can also cause changes in bowel and bladder function.
Disc herniations can affect areas away from the spine. Herniations in the upper part of the thoracic spine can radiate pain and other sensations into one or both arms. If the herniation occurs in the middle of the thoracic spine, pain can radiate to the abdominal or chest area, mimicking heart problems. A lower thoracic disc herniation can cause pain in the groin or lower limbs and can mimic kidney pain.
Diagnosis
How do doctors diagnose the problem?
Diagnosis begins with a complete history and physical examination. Your chiropractic doctor will ask questions about your symptoms and how your problem is affecting your daily activities. These include questions about where you feel pain, if you have numbness or weakness in your arms or legs, and if you are having any problems with bowel or bladder function. Your doctor will also want to know what positions or activities make your symptoms worse or better.
Then the doctor examines you to see which back movements cause pain or other symptoms. Your skin sensation, muscle strength, and reflexes are also tested.
X-rays show the bones. They normally don't show the discs, unless one or more of the discs have calcified. This is significant in the diagnosis of thoracic disc herniation. A calcified disc that appears on X-ray to poke into the spinal canal is a fairly reliable sign that the disc has herniated. It isn't clear why a problem thoracic disc sometimes hardens from calcification, though past injury of the disc is one possibility.
The best way to diagnose a herniated thoracic disc is MRI (magnetic resonance imaging). The MRI machine uses magnetic waves rather than X-rays to show the soft tissues of the body. It gives a clear picture of the discs and whether one has herniated. This machine creates pictures that look like "slices" of the area your doctor is interested in. The test does not require dye or a needle. This test has shown doctors that many people without symptoms have thoracic disc herniations. This has led some doctors to suggest that thoracic disc herniations not causing symptoms are "normal."
Before MRI, doctors relied mainly on myelography to diagnose thoracic disc herniations. By itself, myelography only helps diagnose this condition in about half the cases. Myelography is a kind of X-ray test. A special dye is injected into the space around the spinal canal. The dye shows up on an X-ray. It helps a doctor see if the disc is pushing into the spinal canal.
Computed tomography (CT scan) may be ordered. This is a detailed X-ray that lets doctors see the body's tissue in images that also look like slices. The images provide more information about calcified discs. Doctors may combine the CT scan with myelography. When the CT scan is performed, the myelography dye highlights the spinal cord and nerves. The dye can improve the accuracy of a standard CT scan for diagnosing a herniated thoracic disc.
Doctors rely mostly on MRI for diagnosing thoracic disc herniations. However, they may use myelography and CT scans when preparing to do surgery to fix a herniated thoracic disc.
All content provided by eORTHOPOD® is a registered trademark of Medical Multimedia Group, L.L.C.. Content is the sole property of Medical Multimedia Group, L.L.C.. and used herein by permission.
All materials from eORTHOPOD® are the sole property of Medical Multimedia Group, L.L.C.. and are used herein by permission. eORTHOPOD® is a registered trademark of Medical Multimedia Group, L.L.C..
|